On March 9, the medical journal "The Lancet" published a study titled "Clinical course and risk factors for mortality of adult inpatients with Covid-19 in Wuhan, China: a retrospective cohort study" by Chinese doctors online.
This study, for the first time, described new data on viral shedding, covering 191 patients (137 discharged, 54 died). The median surviving duration of viral shedding was 20 days, but the new coronavirus was detectable in patients who unfortunately died until they died. Among them, the longest shedding time observed by researchers was 37 days.
You can view the original text here:
https://www.thelancet.com/pb-assets/Lancet/pdfs/S014067362305663.pdf
The study was led by Cao Bin, deputy director of the China-Japan Friendship Hospital, and included Liu Zhibo, Ph.D. of Wuhan Jinyintan Hospital.
The study is the latest observation of 191 adult patients diagnosed with new type of coronavirus pneumonia in two hospitals in Wuhan (135 cases at Wuhan Jinyintan Hospital and 56 cases at Wuhan Pulmonary Hospital).
The coverage time was admission on December 29, 2019, and discharge or death before January 31, 2020.
Studies show that viral shedding takes longer than expected for hospitalized patients with new coronavirus pneumonia, but the authors suggest that, given the patient's severe illness in the study, limited samples and genetic material were tested, the true viral shedding duration for all patients Still unclear.
Older age, symptoms of sepsis, and coagulation problems on admission are key risk factors associated with a high risk of death from new coronaviruses.
This new study examines for the first time the risk factors for serious illness and death related to the final discharge or death outcomes of hospitalized adults.
Of the 191 patients, 137 were discharged and 54 died at the hospital. The authors point out that the interpretation of their findings may be limited by the study sample size.
In addition, the authors provide new data on viral shedding, which indicates that the median duration of viral shedding for survivors is 20 days (ranging from 8 to 37 days) and among 54 non-survivors until death. Viruses can be detected.
Although prolonged viral shedding suggests that patients may still be able to transmit the new coronavirus, the authors say that the duration of viral shedding is affected by the severity of the disease and noted that all patients in the study were hospitalized, two-thirds of whom The patient had a severe or major illness.
In addition, the estimated duration of viral shedding is limited by the low frequency of collection of respiratory specimens and the lack of measurable detection of genetic material in the samples.
"In our study, it was found that prolonged shedding of the virus has important guiding significance for the isolation prevention measures and antiviral treatment of patients with newly diagnosed new coronavirus pneumonia infection. However, we need to be clear that there is no Symptom-infected persons should not confuse the virtual shedding time with other self-isolation guidelines, as the guidelines are based on the latency of the virus," explained Cao Bin, deputy director of the China-Japan Friendship Hospital.
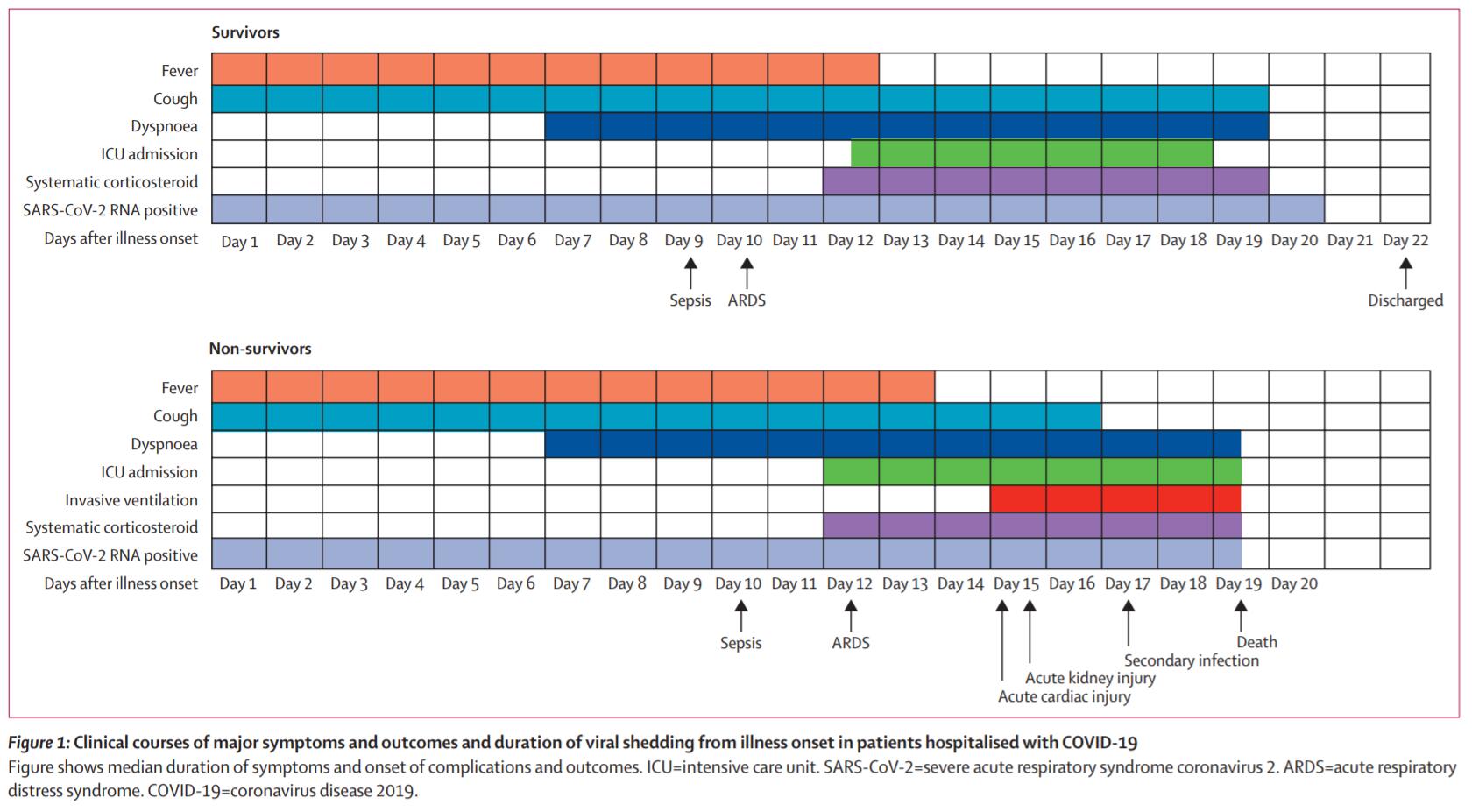
This study describes for the first time a complete picture of the progression of novel coronavirus pneumonia. Survivors had a median fever of about 12 days, similar to non-survivors.
But the cough of the survivors may persist for a long time, and 45% of the survivors will still cough after being discharged from the hospital.
In survivors, dyspnea (shortness of breath) will stop after about 13 days, but will continue until the death of non-survivors.
This study also illustrates when different complications occur, such as sepsis, acute respiratory distress syndrome (ARDS), acute heart injury, acute kidney injury, and secondary infections.
During the study, researchers compared clinical records, treatment data, laboratory results, and demographic data between discharged survivors and non-survivors.
They studied the symptoms during hospitalization, the clinical course of viral shedding and laboratory test results (for example, blood tests, chest X-rays, and CT scans), and used mathematical models to examine the risk factors associated with hospital deaths.
Studies indicate that, on average, patients are middle-aged (median age 56 years), most are male (62%, 119 patients), and about half have underlying chronic disease (48%, 91 patients). It is common to have hypertension (30%, 58 patients) and diabetes (19%, 36 patients).
From the onset, the average discharge time of patients was 22 days, and the average death time was 18.5 days.
Compared with survivors, dead patients are older (mean age 69 vs 52) and have a higher score on sequential organ failure assessment (SOFA), septicemia at admission and blood medication for d-dimer protein Increased concentration (coagulation index).
The authors also noted some limitations of the study, including the exclusion of patients who were still in the hospital after January 31, 2020. The study was restricted to an earlier stage of the epidemic, the patients were relatively sick, and the number of deaths was the true mortality of the new coronavirus pneumonia is not reflected.
They also point out that not all patients have undergone all laboratory tests (such as d-dimer tests) and may therefore underestimate their exact role in predicting in-hospital deaths.
Finally, the lack of effective antiviral drugs, inadequate compliance with standard supportive therapies, high doses of corticosteroids, and the transfer of some patients to the hospital in advanced stages may all lead to poor prognosis in some patients.
Special Report: Fighting The New Coronavirus